Program Philosophy
The School of Nursing responds to the needs of our community in developing the curriculum; and aligns itself with our community service partners in providing educational experiences for the students.
In keeping with the mission of Ventura College, the target population of Ventura College School of Nursing consists of individuals, families, groups, and communities in Ventura County. Ventura is a county composed of an ethnically, economically and demographically diverse population. Refugees, immigrants, and homeless live in this community. The school serves this diverse community of patients who present with health care needs occurring from conception to death and in all stages of human development. Utilization of the surrounding health care facilities provides a rich environment for nursing practice as nurses address the health care problems indigenous to the area. Health care services are available at public and private facilities. Major challenges facing this community include access to affordable health care and high mortality rates for certain populations such as infants and the elderly, substance abusers and the psychiatrically ill without support services.
The nursing education philosophy recognizes that students have individual learning needs, learning styles, readiness, support systems, and cultural and ethnic backgrounds. Learning is a continuous, life-long process that occurs in the affective, cognitive and psychomotor domain, proceeding from simple to complex and enhanced by an environment that motivates the student to apply the theory to practice using critical thinking, evidence-based practice, informatics, clinical simulation experience, patient-centered care, the nursing process, and the clinical judgment model.
The faculty use diverse teaching strategies to meet the varied learning styles and learning needs of our diverse students. Faculty are committed to assisting all students to achieve their professional goals by providing a supportive environment for learning and personal growth in an accessible, inclusive, and equitable learning environment. Student support programs are utilized to assist students in achieving academic success from entry to graduation.
Education of the nurse at the Associate Degree level prepares the individual as an entry level nurse in the profession of nursing. The nurse is educated to provide safe, competent, caring interventions, and patient care management through sound clinical decision making, communication, and leadership. Integrity, respect for the individual, ethical behavior, accountability, and lifelong learning are attributes of the art and science of nursing care.
The faculty believe that nursing as a profession is an art and science as well as practice discipline that responds to society’s health needs in a caring manner in a variety of diverse environments. As a scientific discipline, nursing draws on a discrete body of knowledge that incorporates an understanding of the relationships among nurses, patients, and environments within the context of health, nursing concepts and theories, and concepts and theories derived from the basic sciences, humanities, and other disciplines. The science of nursing is applied in practice through a critical thinking framework known as the nursing process that is composed of assessment, diagnosis, planning, implementation, and evaluation. The steps of the nursing process serve as a foundation for clinical decision-making and evidence-based practice. Nurses use critical thinking to integrate objective data with knowledge gained from an assessment of the subjective experiences of patients and groups, and to apply the best available evidence and research data to the processes of diagnosis and treatment. Nurses use clinical reasoning to respond to the needs of the populations they serve. Nurses develop and communicate strategies to support optimal outcomes that are most appropriate to the patient or situation while being mindful of resources utilization. Nurses continually evaluate the quality and effectiveness of nursing practice and seek to optimize outcomes (American Nurses Association [ANA], 2021.
The art of nursing is based on a framework of unconditional acceptance of the humanity of others, respecting their dignity and worth, while providing compassionate, comforting care. The art and science of nursing are inextricably linked, as a compassionate approach to patient care carries a mandate to provide care competently and within a systems-based practice. Competent care is provided and accomplished through delegated, independent and interdependent practice and through communication as well as collaborative practice involving other colleagues and/or the individuals seeking support or assistance with their healthcare needs (ANA, 2021, p. 5-6).
The distinctive focus of the discipline of nursing is on nursing actions and processes, which are directed toward human beings and take into account the environment in which individuals reside and in which nursing practice occurs. This distinctive focus is reflected in the metaparadigm of nursing, which identifies human beings (patients), the environment, health, and nursing as the matter of interest to nurses (ANA, 2021). In the context of nursing knowledge, these constructs are defined as follows:
Human beings/patients – The recipient of a healthcare service or intervention at the individual, family, community, or aggregate level. Patients may function in independent, interdependent, or dependent roles, and may seek or receive nursing interventions related to disease prevention,
health promotion, or health maintenance, as well as illness and end-of-life care (AACN, 2021, p. 62).
Environment – an open and evolving system consisting of internal and external factors, such as physical, psychological, social, cultural and spiritual influences that affect the life, health, and survival of a person or community. The person interacts and communicates with the environment. The nurse achieves patient outcomes by providing a safe and effective health care environment in order to protect patients, families, groups, and other health care personnel within the context of community.
Health – an experience that is often expressed in terms of wellness and illness and may occur in the presence or absence of disease or injury (ANA, 2021, p. 112).
Nursing – Nursing integrates the art and science of caring and focuses on the protection, promotion, an optimization of health and human functioning; prevention of illness and injury; facilitation of healing; an alleviation of suffering through compassionate presence. Nursing is the diagnosis and treatment of human responses and advocacy in the care of individuals, families, groups, communities, and populations in recognition of the connection of all humanity. (ANA, 2021, p. 112-113).
Organizing Concepts
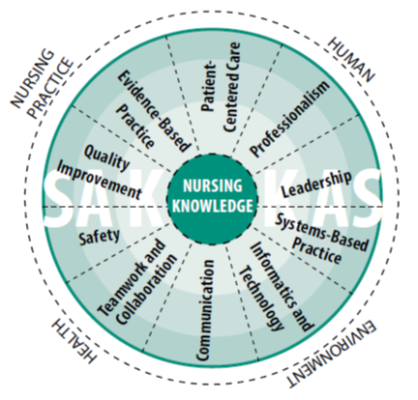
The ten (10) core organizing concepts emanate from the foundation of nursing knowledge. The concepts consist of the following:
• Patient-Centered Care
• Professionalism
• Informatics and Technology
• Evidence-Based Practice
• Leadership
• Systems-Based practice
• Safety
• Communication
• Teamwork and Collaboration
• Quality Improvement
See model.
Ten (10) major organizing concepts with eleven (11) content concepts (categories of health alterations) are integrated in all courses throughout the program including:
1. Alterations in Oxygenation
2. Alterations in Tissue Perfusion
3. Alterations in CNS Regulation
4. Alterations in Immunity
5. Alterations in Tissue Integrity
6. Alterations in Mobility
7. Alterations in Reproduction
8. Alterations in Digestion and Elimination
9. Alterations in Homeostasis
10. Alterations in Mental Health
11. Alterations in Cellular Regulation
Figure 1: The model is a graphic representation of the ten organizing concepts and their relationship to nursing knowledge. In the model, nursing knowledge has been placed at the core to represent how nursing knowledge in its totality reflects the overarching art and science of the nursing profession and discipline. The organizing concepts, which guide nursing curricula and practice, emanate from this central core and include patient-centered care, professionalism, leadership, systems-based practice, informatics and technology, communication, teamwork and collaboration, safety, quality improvement, and evidence-based practice. The order of the concept does not indicate any hierarchy, as all the concepts are of equal importance. The concepts are connected by broken lines because distinction between individual concepts may be blurred; the concepts overlap and are not mutually exclusive. The concepts are similarly connected to the core by a broken line to indicate the reciprocal and continuous relationship between each of the concepts and nursing knowledge.
Adapted from Massachusetts Nurse of the Future 2016
Conceptual Framework
The conceptual framework of the Ventura College Associate Degree Nursing Program is derived from statements in the program philosophy related to four major interdependent nursing concepts: nursing, the person, (patient), the environment and health. Patients are the recipients of nursing care or services and may be individuals, families, groups, communities or populations. Health is an experience that is often expressed in terms of wellness and illness, and may occur in the presence or absence of disease or injury. Environment is an open and evolving system consisting of internal and external factors, such as physical, psychological, social, cultural and spiritual influences that affect the life, health, and survival of a person or community. Nursing is a dynamic profession that uses relevant knowledge from the physical, social and behavioral sciences, as well as the nursing process, as a basis for diagnostic reasoning, clinical decision making and planning the restoration and maintenance of patient health and wellness.
Sub concepts are deduced from the four major concepts and serve to organize the process and the content of the nursing curriculum (p. 9). The sub concepts are called Organizing Concepts and they are: patient-centered care, quality improvement, teamwork and collaboration, professionalism, evidence - based practice, safety, systems based practice, communication, leadership and informatics.
Content Concepts flow from the Organizing Concepts and are integrated into course content as curriculum threads. The Content Concepts represent alterations in: oxygenation, perfusion, CNS Regulation, motility, homeostasis, tissue integrity, elimination, cellular regulation, immunity, reproduction and mental health. These Content Concepts are linked to Associated Content Areas/Systems. For example, the Content Concept, alteration in oxygenation, is linked to the Associated Content Area, the respiratory system.
Alterations continue to thread through the courses as Related Concepts. Related concepts are the health care deviations experienced by patients. For example, an alteration in motility, directs course content to include arthritis and fractures and their effects on the musculoskeletal system.
There are four Integrated Concepts, nutrition, gerontology, pharmacology and pediatrics. Nutrition, gerontology and pharmacology are threaded through all nursing courses and direct the discussion of these content areas as they apply to the alterations studied in each course. Pediatric content is integrated in only one nursing course, the second nursing course. (NS V20).
Content related to the five Organizing Concepts (safety, quality improvement, systems-based practice, leadership and teamwork & collaboration) can be further defined. For example, leadership covers content related to delegation, power & polities and change, while safety covers content related to dosage calculation, nursing skills and patient abuse. The related content for these organizing concepts thread through courses where appropriate. For example, the definition of delegation is introduced in the first nursing course, while students practice delegation in the clinical area in the last nursing course. The Integrated Concepts again thread through these content areas as appropriate.
Content related to the five Organizing Concepts (patient-centered care, professionalism, evidence-based practice, communication and informatics) can be further defined. For example, communication covers content related to therapeutic communication, reporting care and documentation, while patient-centered care covers content related to the nursing process and self-care. The related content for these Organizing Concepts thread through courses where appropriate. For example, an overview of the nursing process is discussed in fundamentals along with a focus on the first two steps of the nursing process, assessment and problem identification. The focus of the second nursing course is planning, and the focus of the third nursing course implementation. Finally, the focus of the last nursing course is evaluation, each course building on the growing expertise of students in the previous steps of the nursing process. The Integrated Concepts again thread through these content areas as appropriate.
The nursing program and curriculum content progress from simple to complex, each course building on the previous ones while introducing new and more complex knowledge. Together, the major concepts, sub concepts and curricular threads form an interactive unified curriculum. The organizing framework guides the establishment of the end of program student learning outcomes (EPSLOs), course student learning outcomes (CSLOs) and the sequencing of course content for the nursing curriculum.
Program Student Learning Outcomes
Graduates of the Ventura College ADN Program will demonstrate the following:
- Provide safe, quality, culturally appropriate, patient-centered care to patients, families, and groups supported by evidence-based clinical decisions and patient preferences in a variety of settings.
- Communicate effectively with patients and members of the inter-professional health care team to provide and coordinate safe, quality, patient-centered care.
- Demonstrate leadership and system management knowledge and skills in the delivery of quality health care to patients while contributing to the effectiveness and efficiency of the work unit.
- Integrate established regulatory (California Nurse Practice Act), legal and ethical principles into standard-based professional nursing practice.
Evidence that graduates have learned the knowledge, skills and ethical basis for nursing practice is not only reflected in student accomplishment of level competencies, but also:
- Performance on the NCLEX licensure examination
- Program completion
- Program satisfaction
- Job placement